Researchers unveil prototype implantable artificial kidney to replace dialysis
By Darren Quick
00:43 September 3, 2010
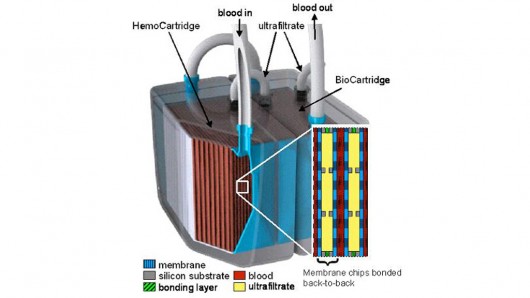
A model of the implantable bioartificial kidney shows the two-stage system
End-stage renal disease, or chronic kidney failure, affects more than 500,000 people per year in the U.S. alone, and currently is only fully treated with a kidney transplant. That number has been rising between five to seven percent per year and with just 17,000 donated kidneys available for transplant last year the waiting list currently exceeds 85,000, according to the Organ Procurement and Transplant Network. Those who can’t secure a kidney for transplant are left reliant on kidney dialysis. An expensive and time consuming process that typically requires three sessions per week, for three to five hours per session, in which blood is pumped through an external circuit for filtration. In a development that could one day eliminate the need for dialysis, researchers have unveiled a prototype model of the first implantable artificial kidney.
The device, which would include thousands of microscopic filters as well as a bioreactor to mimic the metabolic and water-balancing roles of a real kidney, is being developed in a collaborative effort by engineers, biologists and physicians nationwide, led by Shuvo Roy, PhD, in the University of California, San Francisco (UCSF) Department of Bioengineering and Therapeutic Sciences.
The treatment has been proven to work for the sickest patients using a room-sized external model developed by a team member in Michigan. Roy’s goal is to apply silicon fabrication technology, along with specially engineered compartments for live kidney cells, to shrink that large-scale technology into a device the size of a coffee cup. The device would then be implanted in the body without the need for immune suppressant medications, allowing the patient to live a more normal life.
The team has established the feasibility of an implantable model in animal models and plans to be ready for clinical trials in five to seven years.
“This device is designed to deliver most of the health benefits of a kidney transplant, while addressing the limited number of kidney donors each year,” said Roy, an associate professor in the UCSF School of Pharmacy who specializes in developing micro-electromechanical systems (MEMS) technology for biomedical applications. “This could dramatically reduce the burden of renal failure for millions of people worldwide, while also reducing one of the largest costs in U.S. healthcare.”
Aside from the toll taken on human patients resulting from the exhausting schedule, dialysis only replaces 13 percent of kidney function. As a result, only 35 percent of patients survive for more than five years.
The implantable device aims to eradicate that problem with a two-stage system that uses a hemofilter to remove toxins from the blood, while applying recent advances in tissue engineering to grow renal tubule cells to provide other biological functions of a healthy kidney. The process relies on the body’s blood pressure to perform filtration without needing pumps or an electrical power supply.
Roy’s team is collaborating with 10 other teams of researchers on the project, including the Cleveland Clinic where Roy initially developed the idea, Case Western Reserve University, University of Michigan, Ohio State University, and Penn State University.
The first phase of the project, which has already been completed, focused on developing the technologies required to reduce the device to a size that could fit into the body and testing the individual components in animal models. In the second and current phase, the team is working on scaling up the device for humans. The team now has the components and a visual model and is pursuing federal and private support to bring the project to clinical use.
Copyright © gizmag 2003 - 2010 To subscribe or visit go to: http://www.gizmag.com