-
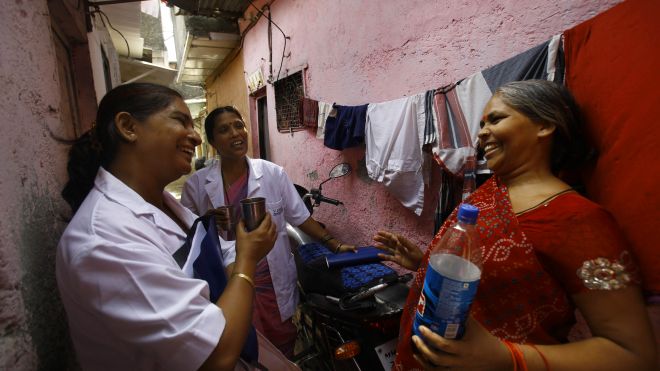
In this Tuesday, May 21, 2013 photo, Usha Devi, right, who was suffering from cervical cancer, talks with health workers from Tata Memorial Hospital in a slum in Mumbai, India. A simple vinegar test slashed cervical cancer death rates by one-third in a remarkable study of 150,000 women in the slums of India, where the disease is the top cancer killer of women. Experts called the outcome amazing and said this quick, cheap test could save tens of thousands of lives each year in developing countries by spotting early signs of cancer, allowing treatment before its too late. Devi, one of the women in the study, says it saved her life. (AP Photo/Rafiq Maqbool)
MUMBAI, India – A simple vinegar test slashed cervical cancer death rates by one-third in a remarkable study of 150,000 women in the slums of India, where the disease is the top cancer killer of women.
Doctors reported the results Sunday at a cancer conference in Chicago. Experts called the outcome "amazing" and said this quick, cheap test could save tens of thousands of lives each year in developing countries by spotting early signs of cancer, allowing treatment before it's too late.
Usha Devi, one of the women in the study, says it saved her life.
"Many women refused to get screened. Some of them died of cancer later," Devi said. "Now I feel everyone should get tested. I got my life back because of these tests."
Pap smears and tests for HPV, a virus that causes most cervical cancers, have slashed cases and deaths in the United States. But poor countries can't afford those screening tools.
This study tried a test that costs very little and can be done by local people with just two weeks of training and no fancy lab equipment. They swab the cervix with diluted vinegar, which can make abnormal cells briefly change color.
This low-tech visual exam cut the cervical cancer death rate by 31 percent, the study found. It could prevent 22,000 deaths in India and 72,600 worldwide each year, researchers estimate.
"That's amazing. That's remarkable. It's a very exciting result," said Dr. Ted Trimble of the National Cancer Institute in the U.S., the main sponsor of the study.
The story of research participant Usha Devi is not an unusual one. Despite having given birth to four children, she had never had a gynecological exam. She had been bleeding heavily for several years, hoping patience and prayers would fix things.
"Everyone said it would go away, and every time I thought about going to the doctor there was either no money or something else would come up," she said, sitting in a tiny room that serves as bedroom, kitchen, bathroom and living room for her entire family.
One day she found a card from health workers trying to convince women to join the study. Devi is in her late 40s and like many poor Indians doesn't know her date of birth. She learned she had advanced cervical cancer. The study paid for surgery to remove her uterus and cervix.
The research effort was led by Dr. Surendra Shastri of Tata Memorial Hospital in Mumbai. India has nearly one-third of the world's cases of cervical cancer — more than 140,000 each year.
"It's just not possible to provide Pap smear screening in developing countries. We don't have that kind of money" or the staff or equipment, so a simpler method had to be found, Shastri said.
Starting in 1998, researchers enrolled 75,360 women to be screened every two years with the vinegar test. Another 76,178 women were chosen for a control, or comparison group that just got cancer education at the start of the study and vouchers for a free Pap test — if they could get to the hospital to have one. Women in either group found to have cancer were offered free treatment at the hospital.
Still, this quick and free cancer screening was a hard sell in a deeply conservative country where women are subservient and need permission from husbands, fathers or others for even routine decisions. Social workers were sent into the slums to win people over.
"We went to every single house in the neighborhood assigned to us introducing ourselves and asking them to come to our health talks. They used to come out of curiosity, listen to the talk but when we asked them to get screened they would totally refuse," said one social worker, Vaishnavi Bhagat. "The women were both scared and shy."
One woman who did agree to testing jumped up from the table when she was examined with a speculum. "She started screaming that we had stolen her kidney," Bhagat said. Another health worker was beaten by people in the neighborhood when women realized they would have to disrobe to be screened.
"There was a sense of shame about taking their clothes off. A lot of them had their babies at home and had never been to a doctor," said one health worker, Urmila Hadkar. "Sometimes just the idea of getting tested for cancer scared them. They would start crying even before being tested."
But screening worked. The quality of screening by health workers was comparable to that of an expert gynecologist, researchers reported. The study was planned for 16 years, but results at 12 years showed lives were saved with the screening. So independent monitors advised offering it to the women in the comparison group.
An ethics controversy developed during the study. The U.S. Office for Human Research Protections faulted researchers for not adequately informing participants in the comparison group about Pap tests for screening. A letter from the agency in March indicated officials seemed to accept many of the remedies study leaders had implemented.
Others defended the study.
"We looked at the ethics very carefully" and felt them to be sound, and visited the project in India, said Trimble of the National Cancer Institute.
Dr. Sandra Swain, a cancer specialist at Medstar Washington Hospital Center, also defended the research. She is president of the American Society of Clinical Oncology, and the research results were presented at that group's meeting in Chicago on Sunday.
"There really was no wrongdoing there," she said. "They have no screening anyway," so there is no standard of care now.
Officials in India already are making plans to expand the vinegar testing to a wider population.
Many poor countries can't afford mammograms for breast cancer screening either. The India study also has been testing breast exams by health workers as an alternative. Preliminary results suggest breast cancers are being found at an earlier stage, but it's too soon to know if that will save lives because not enough women have died yet to compare the groups, said Trimble of the National Cancer Institute.
More progress against cervical cancer may come from last month's announcement that two companies will drastically lower prices on HPV vaccines for poor countries. Pilot projects will begin in Asia and Africa; the campaign aims to vaccinate more than 30 million girls in more than 40 countries by 2020.
©2013 FOX News Network, LLC. All rights reserved.
http://www.foxnews.com/health/2013/06/02/vinegar-cancer-test-saves-lives-india-study-finds/