2015 Dietary Guidelines Include Healthy Revisions, but Still Falls Short for Effective Prevention of Heart Disease
Story at-a-glance −
- The 2015 to 2020 dietary guidelines for Americans is shifting away from focusing on specific nutrients toward a general focus on eating real food, moderating protein consumption and, for the first time, limiting added sugars
- The limit on dietary cholesterol has been removed entirely. This is good news, since dietary cholesterol is actually one of the most important molecules in your body
- They refuse to review recent studies and continue to vilify saturated fat, stating it raises LDL while ignoring that it only increases safe large fluffy LDL particles and actually increases HDL
By Dr. Mercola
On January 7, 2016, the U.S. government released its 2015 to 2020 dietary guidelines 1,2,3,4,5 many of which are steps in the right direction. Perhaps one of the most promising changes is a shift away from focusing on specific nutrients toward a general focus on eating real food.
My main objections are that they still do not consider the hazards of eating too many non-fiber carbs, which can exacerbate insulin and leptin resistance. And they still inaccurately accuse saturated fats of promoting heart disease.
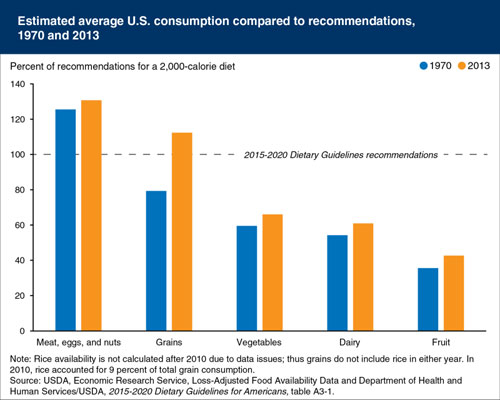
On the upside, they do suggest reducing processed grains overall. The following graph, created by the U.S. Department of Agriculture,6 shows the discrepancies between the 2015-2020 dietary recommendations and what Americans actually consume, comparing statistics from 1970 and 2013.7
Beneficial Changes in the 2015 Dietary Guidelines
Among the beneficial changes brought forth in the 2015 dietary guidelines for Americans, we have:
- New sugar limit: For the first time, the guidelines recommend limiting added sugars to a maximum of 10 percent of your daily calories. Based on a 2,000-calorie-a-day diet, that would equate to about 50 grams of sugar per day, which is still too high if you’re insulin-resistant or diabetic.
I recommend limiting your total fructose intake to 25 grams per day for optimal health, and as low as 15 grams a day if you’re insulin resistant or diabetic.
- Artificial sweeteners should not be used for weight loss. While they say artificial sweeteners such as aspartame are probably OK in moderation, they should not be promoted for weight loss.
This recommendation reflects the overwhelming amount of evidence showing that artificial sweeteners in fact tend to promote weight gain, and have been shown to worsen insulin resistance and metabolic disorders to a greater degree than refined sugar.
- Moderate protein consumption. The new guidelines note that men in particular, tend to eat too much protein.
The guidelines do not go so far as to suggest a limit, however, although it does specify eating 8 ounces of seafood per week which, besides protein, is a source of healthy omega-3 fat.
Nor does it strictly warn against eating processed meats, even though it mentions processed meats have been associated with an increased risk for cardiovascular disease.
For reasons detailed in my previous article, “The Very Real Risks of Consuming Too Much Protein,” I recommend limiting your protein to about one-half gram of high-quality, organic, pastured/grass-fed protein per pound of lean body mass, which for most would be 40 to 70 grams a day.
Eating more high-fat/low-mercury fish in lieu of red meat is one great way to reduce your protein consumption, as fish is far lower in protein than meat. As for processed meats, they have far more risks than benefits, and are best avoided as much as possible.
The International Agency for Research on Cancer, a part of the World Health Organization, has actually classified processed meats as a Group 1 carcinogen, as the evidence strongly shows it can cause colorectal cancer in humans.
- Eat more veggies. The guidelines recommend eating 2.5 cups of a wide variety of vegetables. In my view, you can’t really overdo it when it comes to vegetables, as they’re very low in calories, and supply much needed fiber and prebiotics that nourish beneficial gut bacteria.
Good News: Limit on Dietary Cholesterol Has Been Removed
For the past four decades, the U.S. government has warned that eating cholesterol-rich foods, such as eggs, would raise LDL cholesterol in your bloodstream and promote heart disease. Alas, decades’ worth of research has utterly failed to demonstrate this correlation.
Now, finally, the Dietary Guidelines Advisory Committee has addressed this scientific vacuum, announcing that “cholesterol is not considered a nutrient of concern for overconsumption.”8
In the past, the guidelines suggested a limit of 300 milligrams (mg) per day; the equivalent of about two eggs. Now, the limit on dietary cholesterol has been removed entirely. This is good news, since dietary cholesterol is actually one of the most important molecules in your body.
Cholesterol plays an important role in brain health and memory formation, and is indispensable for the building of cells and the production of stress and sex hormones, as well as vitamin D. (When sunlight strikes your bare skin, the cholesterol in your skin is converted into vitamin D.)
Eggs are a healthy source of cholesterol, provided you buy high-quality eggs, meaning organic and pasture raised. The Cornucopia Institute has created an egg scorecard,9 based on 28 organic criteria, to help you select eggs of the highest quality possible.
Bad News: Saturated Fat Myth Remains
Unfortunately, they still do not retract their previous misinformation and do not tell the truth about saturated fat. Insisting that it raises LDL, while ignoring that it only raises safe fluffy LDL particles, they still omit the very important fact that it actually increases HDL.
This is surprising, considering all the evidence. For example, a 2014 meta-analysis10 published in the Annals of Internal Medicine (which included data from 76 studies and more than a half-million people) found that those who consume higher amounts of saturated fat have no more heart disease than those who consume less.
Moreover, those who ate higher amounts of unsaturated fat, including both (healthy) olive oil and (unhealthy) corn oil — both of which are recommended over saturated fats — did NOT have lower incidence of heart disease.
Another meta-analysis11 published in the British Medical Journal last year also failed to find an association between high levels of saturated fat in the diet and heart disease. Nor did they find an association between saturated fat consumption and other life-threatening diseases like stroke or type 2 diabetes.
Saturated Fat Recommendations Do Far More Harm Than Good
Despite such findings, the updated dietary guidelines still recommend limiting both trans fats (which are indeed harmful) and saturated fat (which is not) to less than 10 percent of your daily calories. This is a far cry from what most people probably need for optimal health. Saturated fats not only are essential for proper cellular and hormonal function, but also provide a concentrated source of energy in your diet.
If you’re insulin-resistant, which most Americans are, then you’d likely benefit from getting as much as 50 to 80 percent of your daily calories from healthy fats. I personally consume about 75 percent of my diet as healthy fat.
For weight loss, they also recommend sticking to low- and non-fat dairy, which I believe is a serious mistake. Low-fat recommendations do more harm than good across the board, but it may be particularly counterproductive if you’re trying to lose weight. In fact, mounting evidence clearly shows that a high-fat, low-carb diet can be exceptionally effective for weight loss — provided you’re eating the right kinds of fats.
For example, research from Johns Hopkins University School of Medicine shows low-carb, high-fat diets promote faster weight loss than a low-fat diet. Low-carb dieters lost 10 pounds in 45 days, while the low-fat dieters needed 70 days to lose the same amount of weight.
Summary of Heart Healthy Diet
To break it down into simple terms, to protect your heart health you need to address your insulin and leptin resistance, which is the result of eating a diet too high in sugars and grains (non-fiber carbs). To safely and effectively reverse insulin and leptin resistance, thereby lowering your heart disease risk, you need to:
- Eat REAL food, ideally as close to their natural state as possible. Avoid processed foods and other sources of refined sugar and processed fructose, and limit non-fiber carbs to under 50 grams a day.
- Focus your diet on whole foods, ideally organic, and replace the grain carbs with:
- Large amounts of vegetables
- Low-to-moderate amounts of high-quality protein (think organically raised, pastured animals and high-fat/low-mercury fish, such as wild Alaskan salmon, anchovies, and sardines)
- As much high-quality healthy fat as you want (saturated and monounsaturated from animal and tropical oil sources). Sources of healthy fats that you'll want to add to your diet include the following:
Organic seeds Coconuts, and coconut oil (for all types of cooking and baking), MCT Oil Butter made from raw grass-fed organic milk Raw nuts, such as macadamias and pecans Organic pastured egg yolks Avocados Grass-fed meats Palm oil Raw cacao nibs
Flawed Cholesterol Treatment Guidelines Turn Healthy People Into Statin Users
According to the U.S. cholesterol treatment guidelines, issued in 2013, if you answer "yes" to ANY of the following four questions, your treatment protocol calls for a statin drug:
- Do you have heart disease?
- Do you have diabetes? (either type 1 or type 2)
- Is your LDL cholesterol above 190?
- Is your 10-year risk of a heart attack greater than 7.5 percent?
Your 10-year heart attack risk involves the use of a cardiovascular risk calculator,12 which researchers have warned may overestimate your risk by anywhere from 75 to 150 percent13 — effectively turning even very healthy people at low risk for heart problems into candidates for statins. The guideline also does away with the previous recommendation to use the lowest drug dose possible and instead basically focuses all the attention on statin-only treatment and at higher dosages.
While shifting attention to LDL cholesterol rather than total cholesterol is a step in the right direction, the guidelines still ignore the density of the lipoproteins. The division into HDL and LDL is based on how the cholesterol combines with protein particles. LDL and HDL are lipoproteins — fats combined with proteins. Cholesterol is fat-soluble, and blood is mostly water. For it to be transported in your blood, cholesterol needs to be carried by a lipoprotein, which is classified by density.
Large fluffy LDL particles are not harmful. Only small dense LDL particles can potentially be a problem, as they can squeeze through the lining of your arteries. If they oxidize, they can cause damage and inflammation. So, you could potentially have an LDL level of 190, but still be at low risk, if your LDLs are large, and your HDL to total cholesterol ratio is above 24 percent. And remember, saturated fat increases your HDL.
Five Reasons to Avoid Statin Drugs
So, while the dietary guidelines no longer focus on reducing dietary cholesterol to protect your heart, and the cholesterol treatment guidelines have stopped using total cholesterol as a measure of heart disease risk (honing in on elevated LDL cholesterol instead), we’re still far off the mark when it comes down to how to best prevent heart disease.
Refined sugar and processed fructose are in fact the primary drivers of heart disease, so that’s where the focus needs to be; not on driving down your cholesterol with the aid of a statin drug (and/or avoiding healthy saturated fats in your diet). The ONLY subgroup that might benefit from a statin are those born with a genetic defect called familial hypercholesterolemia, as this makes them resistant to traditional measures of normalizing cholesterol.
There are many great reasons why you should NOT take a statin drug unless you have this genetic defect, including but not limited to the following five:
- They don't work as advertised. A 2015 report14 published in the Expert Review of Clinical Pharmacology concluded that statin advocates used a statistical tool called relative risk reduction (RRR) to amplify statins’ trivial beneficial effects. If you look at absolute risk, statin drugs benefit just 1 percent of the population. This means that out of 100 people treated with the drugs, one person will have one less heart attack.
- They deplete your body of CoQ10. Statins block HMG coenzyme A reductase in your liver, which is how they reduce cholesterol. But this is also the same enzyme that makes CoQ10, which is an essential mitochondrial nutrient that facilitates ATP production.
- They inhibit the synthesis of vitamin K2 — a vitamin that protects your arteries from calcification.
- They reduce ketone production.15 If you take CoQ10 while on statins you did not solve the problem, as the same enzyme also inhibits your liver’s ability to produce ketones, which are not only water-soluble fat nutrients important for tissue health but also important molecular signaling molecules.
- Because of Nos. 2, 3 and 4 they increase your risk for other serious diseases, including:
- Cancer. Research16 has shown that long-term statin use (10 years or longer) more than doubles women's risk of two major types of breast cancer: invasive ductal carcinoma and invasive lobular carcinoma.
- Diabetes. Statins have been shown to increase your risk of diabetes via a number of different mechanisms, two of which include increasing your insulin resistance, and raising your blood sugar.
- Neurodegenerative diseases
- Musculoskeletal disorders and motor nerve damage. Research17 has shown that statin treatment lasting longer than two years causes “definite damage to peripheral nerves.”
- Cataracts
New Class of Cholesterol Drugs May Be Even More Harmful Than Statins
Also beware of a newer class of cholesterol absorption inhibitors called PCSK9 Inhibitors.18 PCSK9 is a protein that works with LDL receptors that regulate LDL in the liver and release LDL cholesterol into the blood. The inhibitors work by blocking that protein and thus having less LDL to circulate in the blood; in clinical trials, these drugs lowered LDLs by about 60 percent.
While these drugs are being touted as the answer for those who cannot tolerate some of the side effects of the other drugs, such as severe muscle pain, trials have already discovered that PCSK9 inhibitors can produce “neurocognitive effects,” with some patients experiencing confusion and attention deficits.19 There’s evidence suggesting these drugs may actually be even more dangerous than statins.
Making Sense of Your Cholesterol Levels, and Assessing Your Heart Disease Risk
Embed this infographic on your website:
Click on the code area and press CTRL + C (for Windows) / CMD + C (for Macintosh) to copy the code.
As a general rule, cholesterol-lowering drugs are not required or prudent for the majority of people — especially if high cholesterol and longevity run in your family. Also keep in mind that your overall cholesterol level says very little about your risk for heart disease.
For more information about cholesterol and what the different levels mean, take a look at the infographic above. As for evaluating your heart disease risk, the following tests will provide you with a far more accurate picture than your total cholesterol or LDL level alone:
HDL / Cholesterol ratio HDL percentage is a very potent heart disease risk factor. Just divide your HDL level by your total cholesterol. That percentage should ideally be above 24 percent Triglyceride/HDL ratio You can also do the same thing with your triglycerides and HDL ratio. That percentage should be below 2 NMR LipoProfile Large LDL particles are not harmful. Only small dense LDL particles can potentially be a problem, as they can squeeze through the lining of your arteries. If they oxidize, they can cause damage and inflammation.
Some groups, such as the National Lipid Association, are now starting to shift the focus toward LDL particle number instead of total and LDL cholesterol, in order to better assess your heart disease risk. Once you know your particle size numbers, you and your doctor can develop a more customized program to help manage your riskYour fasting insulin level Any meal or snack high in carbohydrates like fructose and refined grains generates a rapid rise in blood glucose and then insulin to compensate for the rise in blood sugar.
The insulin released from eating too many carbs promotes fat accumulation and makes it more difficult for your body to shed excess weight. Excess fat, particularly around your belly, is one of the major contributors to heart diseaseYour fasting blood sugar level Studies have shown that people with a fasting blood sugar level of 100 to 125 mg/dl had a nearly 300 percent increase higher risk of having coronary heart disease than people with a level below 79 mg/dl Your iron level Iron can be a very potent oxidative stress, so if you have excess iron levels you can damage your blood vessels and increase your risk of heart disease. Ideally, you should monitor your ferritin levels and make sure they are not much above 80 ng/ml.
The simplest way to lower them if they are elevated is to donate your blood. If that is not possible you can have a therapeutic phlebotomy and that will effectively eliminate the excess iron from your body
How to Lower Your Risk for Heart Disease Without Drugs
Heart disease is predominantly the end result of unhealthy lifestyle choices, and cholesterol-lowering medications are far from being magic bullets to lower your risk of dying from heart disease — especially when you consider that your body needs cholesterol for optimal functioning.
In a nutshell, preventing cardiovascular disease involves reducing chronic inflammation in your body. Proper diet, exercise, sun exposure, and grounding to the earth are cornerstones of an anti-inflammatory lifestyle. For more details on how to naturally reduce your risk of heart disease, please review the following 10 heart-healthy strategies:
Eat REAL FOOD. Replace processed foods (which are loaded with refined sugar and carbs, processed fructose, and trans fat — all of which promote heart disease) with whole, unprocessed or minimally processed foods, ideally organic, and/or locally grown. Avoid meats and other animal products such as dairy and eggs sourced from animals raised in confined animal feeding operations (CAFOs). Instead, opt for grass-fed, pastured varieties, raised according to organic standards. Limit your protein intake to one half gram of protein for every pound of lean body mass which is about 40 to 70 grams for most people. Eliminate no-fat and low-fat foods, and increase consumption of healthy fats. Those with insulin resistance would likely benefit from consuming 50 to 85 percent of their daily calories from healthy saturated fats, such as avocados, butter made from raw grass-fed organic milk, raw dairy, organic pastured egg yolks, coconuts and coconut oil, unheated organic nut oils, raw nuts, and grass-fed meats.
No- or low-fat foods are usually processed foods that are high in sugar, which raises your small, dense LDL particles.Balancing your omega-3 to omega-6 ratio is also key for heart health, as these fatty acids help build the cells in your arteries that make the prostacyclin that keeps your blood flowing smoothly.
Omega-3 deficiency can cause or contribute to very serious health problems, both mental and physical, and may be a significant underlying factor of up to 96,000 premature deaths each year. For more information about omega-3s and the best sources of this fat, please review this previous article.You also need the appropriate ratios of calcium, magnesium, sodium, and potassium, and all of these are generally abundant in a whole food diet. To get more fresh vegetables into your diet, consider juicing. Optimize your vitamin D level. Some researchers, like Dr. Stephanie Seneff, believe optimizing your vitamin D level through regular sun exposure, opposed to taking an oral supplement, may be key to optimizing your heart health. If you do opt for a supplement, you also increase your need for vitamin K2. Optimize your gut health. Regularly eating fermented foods, such as fermented vegetables, will help reseed your gut with beneficial bacteria that may play an important role in preventing heart disease and countless other health problems. Quit smoking and reduce your alcohol consumption. Exercise regularly. Exercise is actually one of the safest, most effective ways to prevent and treat heart disease. In 2013, researchers at Harvard and Stanford reviewed 305 randomized controlled trials, concluding there were "no statistically detectable differences" between physical activity and medications for heart disease.
High-intensity interval training, which requires but a fraction of the time compared to conventional cardio, has been shown to be especially effective. Exercise is one of the most important stimulants of mitochondrial biogenesis.Pay attention to your oral health. There's convincing evidence linking the state of your teeth and gums to a variety of health issues, including heart disease. In one 2010 study,20 those with the worst oral hygiene increased their risk of developing heart disease by 70 percent, compared to those who brush their teeth twice a day. Avoid statins, as the side effects of these drugs are numerous, while the benefits are debatable. If you are taking statins for any reason it is imperative to take Coenzyme Q10. I believe the best is the reduced form called Ubiquinol.
© Copyright 1997-2016 Dr. Joseph Mercola. All Rights Reserved.